
For people at high risk of breast cancer, timely and accurate screening can be lifesaving, helping doctors to find cancer earlier and tailor treatments more precisely. At MUSC Hollings Cancer Center, breast imaging is often the first step in a patient’s cancer journey, helping care teams to diagnose disease, plan treatment and monitor response.
Mammography is the gold standard for breast cancer screening and detection. Breast MRI is recommended for patients with newly diagnosed breast cancer or as an additional screening to supplement mammography for patients who are at high risk for breast cancer. But not everyone can safely undergo an MRI – leaving some patients with limited options.
Now, MUSC Health is closing that gap.
At MUSC Health’s West Ashley Medical Pavilion, patients who cannot safely undergo a breast MRI can now receive contrast-enhanced mammography, an advanced imaging technique that offers greater sensitivity than a standard mammogram when an MRI is not an option.
“This is about filling a gap,” said Rebecca Leddy, M.D., medical director of breast imaging at MUSC Health-Charleston Division. “For patients for whom an MRI would be recommended, like those with a new cancer diagnosis, but who couldn’t get an MRI, we didn’t have an imaging option to offer them before. Now we do.”
What is contrast-enhanced mammography?
Contrast-enhanced mammography builds on a traditional mammogram by adding a special dye to help doctors to see the breast more clearly. The dye, which is also used in CT scans, highlights areas in the breast that may be different from healthy tissue.
During a contrast-enhanced mammogram, patients receive breast compression, as they would during a standard mammogram, while also receiving the dye through an IV. After it is injected, the dye travels through the bloodstream and is absorbed differently in different tissues. Images taken shortly after the dye is administered allow radiologists to see whether areas of breast tissue take up the dye, which can be a hallmark of many cancers.
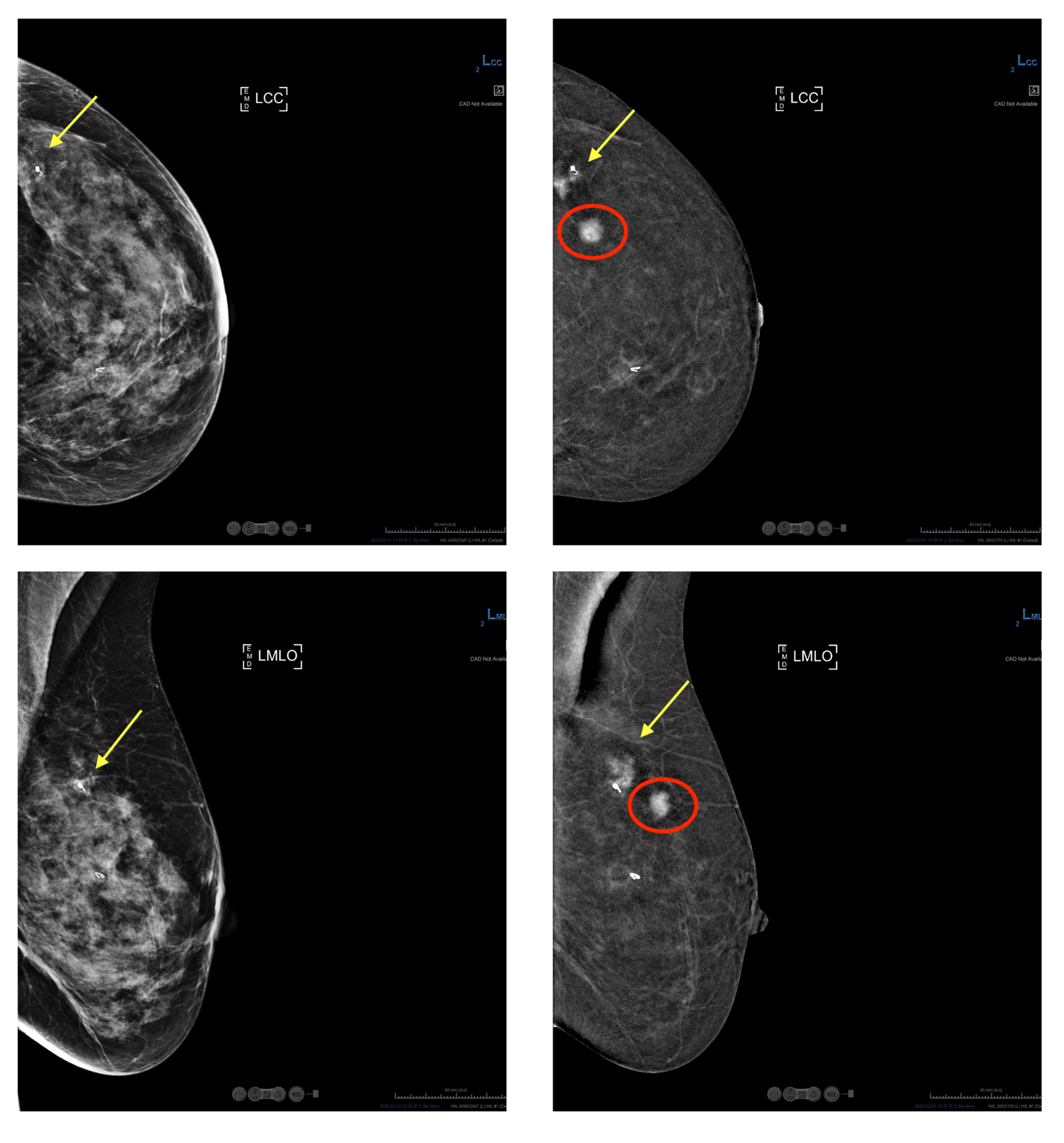
“The concept is similar to an MRI,” Leddy explained. “Cancer cells often take up contrast dye differently than healthy tissue, so this helps us spot areas that warrant a closer look.”
Who should – and should not – get contrast-enhanced mammography?
Contrast-enhanced mammography is used on a case-by-case basis for patients who need more advanced imaging but cannot safely undergo an MRI. These include people who have:
- A pacemaker or other implanted device that is not MRI-safe.
- An allergy to the gadolinium contrast used in an MRI.
- Severe claustrophobia that cannot be managed with medication.
“They’re not meant to be interchangeable,” Leddy said. “If someone can get an MRI, that’s still what they should be receiving.”
Breast MRI remains the preferred imaging test for people at high risk for breast cancer, typically defined as a lifetime risk greater than 20%, as well as for patients newly diagnosed with breast cancer who need imaging to assess the extent of their disease.
“With an MRI, we get more information,” Leddy said. “We can look at changes over time in the scans, see deeper soft tissues and assess the chest wall and lymph nodes. Mammography focuses just on the breast itself.”
On the other hand, some people are not candidates for contrast-enhanced mammography. Because the test uses iodinated contrast that is filtered out by the kidneys, people with significant kidney disease or a history of allergic reaction to CT contrast may not be eligible. Patients with breast implants are not candidates because the device’s positioning and imaging limitations can affect image quality.
What can patients expect during contrast-enhanced mammography?
Contrast-enhanced mammography is reported to feel much like a combination of a mammogram and a CT scan.
“You’re still standing, still having breast compression, still being positioned for the mammogram,” Leddy said. “The difference is that you also have an IV for the contrast.”
Some people report a brief warm sensation or the feeling of needing to use the restroom when the contrast is injected – a normal and temporary effect. There is no need to fast or prepare beforehand, though kidney function may be checked in people over 65 or with known kidney concerns.
This shows that MUSC Health is really paying attention to patient needs. We recognized that there was a group of patients we weren’t fully able to serve, and we worked to find a better option for them.
Because contrast-enhanced mammography is currently approved as a diagnostic tool, rather than a routine screening test, it is used thoughtfully and selectively. Radiologists at MUSC Health review each case to ensure that the test is appropriate.
“We’re emphasizing collaboration,” Leddy said. “If a doctor orders this, we want to make sure it truly makes sense for that patient.”
She is enthusiastic about the new technology – but with an important caveat.
“I’m excited that we have another tool,” she said. “But I’m also very clear that this does not replace MRI. It’s about expanding options without lowering standards.”
Leddy sees contrast-enhanced mammography as an important step toward more personalized care – recognizing that not all patients fit neatly into standard imaging pathways.
“This shows that MUSC Health is really paying attention to patient needs,” she said. “We recognized that there was a group of patients we weren’t fully able to serve, and we worked to find a better option for them.”
For patients wondering whether contrast-enhanced mammography might be right for them, Leddy encourages them to start with a conversation.
“Talk to your doctor,” she said. “Your provider can work with the radiologist to determine what imaging approach is safest and most appropriate for you.”
Featured in this story

Rebecca J. Leddy, M.D.
Professor, Department of Radiology and Radiological Science
Dr. Rebecca Leddy received her Bachelor of Science and Medical Doctorate from the University of Florida. Dr. Leddy then completed a diagnostic radiology residency at Emory University in Atlanta, Georgia. She is certified by the American Board of Radiology. Dr. Leddy completed a fellowship in breast imaging radiology at the Medical University of South Carolina (MUSC) and joined the faculty at MUSC in 2010. Dr. Leddy is currently a Professor in Radiology at MUSC, the Medical Director of Breast Imaging at MUSC Charleston, MUSC Department of Radiology Breast Imaging Section Chief, and the MUSC Breast Imaging Fellowship Director. Dr. Leddy has presented nationally on her breast imaging research. Her interests are in breast education and in healthcare disparities. She resides in Charleston with her husband, three kids, and dog.





